Modern Responses to Mental Illness
Executive Summary
The failure of our mental health institutions to adequately treat the severely mentally ill (SMI) is exploding onto American streets. Decades of misguided policy and advocacy, ostensibly in support of America’s vulnerable SMI community, have forced thousands of mentally ill individuals into homelessness or prisons. Failure to treat serious mental illness has imperiled American streets, further stressed an overrun American justice system, and cost American taxpayers millions of dollars. Dramatic change is needed.
President Trump, through Executive Order 14321, Ending Crime and Disorder on America’s Streets, has instructed governors and state agencies to direct their attention towards the spiraling mental health problem in America. This white paper examines the origins and consequences of this crisis, which dates back to the Community Mental Health Act of 1963, to provide legislators with a deeper understanding of the history of our mental health institutions and the scope of their inadequacies. To address the issues highlighted, such as the inability of many states to civilly commit severely mentally ill and potentially dangerous residents and the failures of the Protection and Advocacy for Individuals with Mental Illness (PAIMI) advocacy groups, States could implement the following measures:
- Expand civil commitment powers
Broaden “dangerousness” definitions beyond imminent harm to include long-term deterioration, homelessness risk, and substance disorders; expand civil commitment laws. - Reorganize disability rights groups
Reorganize PAIMI advocacy groups, bar inadequately trained staff from treatment advocacy, and reassess funding towards advocacy groups opposed to treatment. - Increase psychiatric bed capacity
Build infrastructure to increase the current bed capacity averages to 30-60 beds per 100,000 residents.
Introduction
The modern mental health system is neither designed nor prepared to properly care for America’s seriously mentally ill. President Trump’s Executive Order 14321, Ending Crime and Disorder on America’s Streets, seeks to challenge the mental health industrial complex and rectify America’s broken mental health system.
The problems surrounding America’s mental health apparatus largely stem from the Community Mental Health Act of 1963, which shifted the focus of federal funding towards mental health centers and away from mental health institutions.1 The laudable goals of the Community Mental Health Act, which sought to rectify the abuses of mental health institutions, failed to replace institutions with the sort of well-organized structure needed to address the complex long-term needs of the severely mentally ill.2 A fragmented, poorly planned procession of for-profit, non-profit, and governmental agencies has risen as a result of deinstitutionalization.3-5
The modern mental health apparatus is a decoupled system focusing on more treatable behavioral health conditions like mild depression, anxiety, and trauma, at the expense of individuals who have the most significant impact on the nation’s jails, prisons, emergency rooms, and homeless population.6
The impact on the severely mentally ill has been extreme. Conservative estimates place 20% of the total prison population as severely mentally ill. The severely mentally ill homeless population has doubled from 60,000 in 1984 to over 137,000 in 2023.7–8 The suicide rate among the severely mentally ill is reported at 312.8 per 100,000 compared to 14.1 per 100,000 in the general population.9–10 However, the most significant impact is arguably in the nation’s emergency rooms, where psychiatric bed usage for the severely mentally ill has risen from 4.37 million in 1992 to over 13.2 million in 2018.11–12

Government agencies and behavioral health providers have had 50 years to fix the broken system and address the national crisis represented by the lack of care for the severely mentally ill and have failed to answer the call. This brief explains the key deficiencies of America’s mental health system and identifies areas of focus for legislators looking to implement President Trump’s mental health agenda.
Involuntary Treatment
Civil commitment is the legal process through which a severely mentally ill individual is court-ordered into treatment. Across the nation, there is a broad range of civil commitment laws, practices, and policies, reflecting a disunified public opinion towards civil commitment. Many people view involuntary commitment as a punishment, calling into question mental health’s categorization as a disease and arguing that the mentally ill are not violent, and therefore do not deserve to be “punished” by civil commitment.13–14
This perspective is as dangerous as it is naïve and short-sighted. The use of involuntary commitment can be essential in preventing psychiatric and physical deterioration, harm, and distress leading to suicide. It is invaluable in helping individuals achieve stability. Withholding involuntary civil commitment as an option deprives the seriously mentally ill of a potentially lifesaving response.15 In recent years, numerous research studies have examined outcomes associated with nonadherence to prescribed medications and untreated psychosis.16–17 These studies chronicle the severe adverse effects of medication noncompliance and recurrent psychosis for extended time periods, which include brain changes that impair thinking and reasoning. More importantly, symptoms become more resistant to antipsychotic treatment, leading to the need for higher medication doses and increased side effects.18 Further, increased social withdrawal and loss of motivation, in some with histories of violent behavior, increases in these behaviors, increased hospitalizations, and early death, often by suicide, have all been associated with treatment noncompliance.19,20,21 To sum it up, in the name of liberty, we are condemning those with serious mental illness to incapacitation, worsened illness, and early death.
The inability to utilize civil commitment laws to assist the mentally ill lies in inconsistencies around the definition of dangerousness. Court decisions to civilly commit revolve around how dangerous a severely mentally ill person could be if left untreated. This definition varies across states and jurisdictions, often creating a barrier to civil commitment.
Dangerousness: The Legal Bedrock of Involuntary Commitment
The concept of dangerousness is foundational to involuntary civil commitment policies. The idea of dangerousness exists on a continuum, with varying interpretations in both clinical and legal contexts. While both frameworks aim to assess risk and prevent harm, they differ substantially in scope, intent, and application.
In clinical psychology and psychiatry, dangerousness is assessed as a prospective judgment about an individual’s capacity to cause harm to self or others. Psychologists cite an individual’s propensity to cause physical or psychological harm to themselves or others.22 Conversely, psychiatrists have adopted a more expansive definition that includes engaging in harmful behavior due to a mental disorder.23 This definition encompasses not only overt threats or actions, but also patterns of behavior that indicate an increasing risk or deterioration. According to Stanislaus (2013), clinicians consider a wide range of factors:

Clinical dangerousness may include “behaviors that violate social norms or pose a threat to the social order,” such as aggression, impulsivity, or criminality—even if they don’t yet constitute imminent harm.25 In this context, dangerousness is not limited to immediate threats, but is instead seen as a dynamic, escalating risk that can be influenced by treatment, environment, and insight.
The legal system has a much narrower definition of dangerousness, emphasizing imminence, specificity, and severity of harm as requirements for civil commitment.26 Legal dangerousness refers to a condition where there is an imminent threat of substantial physical harm to oneself or others, often demonstrated by a recent act, attempt, or credible threat. It is used to justify the deprivation of liberty through involuntary commitment to a hospital. We emphasize that, unlike the broader, subjective clinical interpretation, the legal standard:
- It is rooted in police power and constitutional due process, not just medical necessity.
- Requires objective evidence, such as recent behavior, to justify confinement.
- Must be narrowly applied to prevent overreach and stigmatization of individuals with mental illness.27
According to the Substance Abuse and Mental Health Services Administration (SAMHSA), civil commitment generally requires: A diagnosed mental illness, a refusal or inability to seek voluntary treatment, and a demonstration of imminent risk.28 However, civil commitment decisions often hinge on narrowly construed definitions of dangerousness, emphasizing imminence and specificity of harm. The language varies by jurisdiction, but most require evidence that a person:
- Poses a clear and present danger to themselves or others
- Is likely to suffer serious harm without intervention
- Is gravely disabled due to mental illness.
Nationally speaking, statutes differ on the inclusion of:
- Past dangerous behavior
- Potential future risk
- Severe deterioration from mental illness
- Substance use disorder/Alcohol use disorder
For example, California’s Lanterman-Petris-Short Act allows for 72-hour holds based on danger to self, others, or grave disability.29 New York’s Kendra’s Law permits court-ordered outpatient treatment for individuals with a history of non-compliance and hospitalization, even if not currently dangerous.30 Some states, however, require imminence—meaning harm must be likely to occur in the immediate future, which can prevent proactive intervention in cases of chronic decline.
Criticisms of Using a Dangerousness Standard to Civilly Commit
Difficulties arise when using dangerousness as a legal standard to predict future dangerousness and balance civil liberties. Psychiatrists face pressure to balance public safety and individual autonomy, and tools for risk assessment are imprecise.31 Clinicians evaluate a combination of historical factors such as past violence or suicide attempts, clinical indicators like psychosis, impulsivity, or substance use, and contextual elements such as access to weapons, homelessness, or recent stressors.
The emphasis on defining dangerousness reflects society’s concern for safety while simultaneously undermining preventative care. Many individuals deteriorate until they meet strict legal thresholds of imminent harm, resulting in criminal justice involvement, even when early intervention could have prevented harm.32 Some argue for a broader definition of dangerousness that includes:33
- Long-term physical and psychiatric deterioration
- Risk of chronic homelessness or exploitation
- Hospitalizations, homelessness, or incarcerations due to untreated illness
- The inclusion of substance use disorder and alcohol use disorder
- Consequences of an Ambiguous “Dangerousness” Standard
The consequences of poorly defined standards of dangerousness are reflected in the growing proportion of mentally ill individuals in America’s prisons. The severely mentally ill are rarely aware of their condition.34 Failure to seek treatment causes further deterioration of the mental state. Disability rights advocates call the refusal of mental health treatment to prevent deterioration into criminality a ‘civil right,’ simultaneously recognizing the disability while rejecting the idea that severe mental illness is a medical condition that requires treatment.35 The World Health Organization states that a mental health issue should never be a reason to negate a person’s rights or exclude them from the treatment plan.36 This, however, does not address the severely mentally ill, who have been shown to lack insight into their needs, leading to a worsening disability.37 The severely mentally ill are lumped together with easier-to-treat behavioral health patients based on an unreasonable standard of dangerousness.38 The number of incarcerated severely mentally ill individuals has risen steadily since the 1970s, while the use of civil commitment and psychiatric hospitals has steadily decreased.39
Currently, there are 1,829,000 adults incarcerated in America.40 Estimates range from 20% to 60% of the incarcerated population suffering from severe mental illness.41–42 Using the more conservative 20% of the jail population estimated at 550,000 and the 1,071,000 inmates in state prisons, along with the Federal Register’s estimate for an average yearly incarceration cost of $42,672, the expense of incarcerating the seriously mentally ill exceeds $15 billion yearly.43 This data shows that half (50.2%) of prison inmates report being diagnosed with a severe mental illness, with significant portions reporting bipolar disorder, major depression, and schizophrenia.44 This is approximately 10 times the number within the general population with serious mental illness.45 Further, the National Alliance on Mental Illness’s (NAMI) findings on lifetime mental illness correlate with the deinstitutionalization movement, disability rights movement, and the reduced use of civil commitment to the expansion of the overall prison population.46–47

The Problem of the Mentally Ill Criminal
In the absence of sufficient resources dedicated to treating the mentally ill, hospitals have developed an alternative method called Emergency Department (ED) Boarding. ED boarding occurs when someone with a mental or substance use disorder needs an inpatient level of care, but no inpatient beds are available. It has been estimated that of the 136 million ED visits yearly, 610% are psychiatric, and 21.5% of these individuals will require ED boarding. At an average cost of $2,264, at least $6.62 billion yearly is wasted on subjecting those with mental health conditions to a clinical setting not equipped to meet their needs.48 The mentally ill are frequently warehoused through ED boarding while waiting for a bed in a proper facility to open.
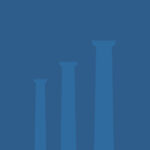
The Treatment Advocacy Center’s 2024 report shows that the optimal number of psychiatric beds is between 30 and 60 per 100,000 residents.49 The Substance Abuse and Mental Health Services Administration (SAMHSA) reported 18 psychiatric beds per 100,000 in 2022, reflecting a severe shortfall in the number of beds needed to treat the severely mentally ill in American society. Some states are worse—Minnesota has only 4.3 beds per 100,000 residents. In 2021, the Treatment Advocacy Center reported 184,00 severely mentally ill Minnesota residents with only 243 hospital beds available. A further breakdown of the SAMHSA report shows that 2,352 of 9,586 programs nationwide focus on specific client groups, particularly those involved with the criminal justice system.
Regarding psychiatric hospitals, SAMHSA reported a total of 39,865 mental health treatment clients held for a 24-hour period. 72% were in private hospital settings. Of those patients within 24-hour care, 44% in the public hospital setting were there as involuntary forensic patients, 40% were involuntary non-forensic, and the remaining 16% were voluntary patients.
Protection and Advocacy for Individuals with Mental Illness
The Protection and Advocacy for Individuals with Mental Illness (PAIMI) statute was first established in 1986 in response to Congress’s finding of widespread abuse and neglect in state-run psychiatric facilities.50 Modeled after the Developmental Disabilities Act, early reformers were focused on the physical conditions of these institutions as well as the growing legal challenges to civil commitment laws. The Federal Register Volume 62, Number 199 specified that Protection and Advocacy agencies were required to protect and advocate for the rights of persons with mental illness, and investigate reports of abuse and neglect in facilities that care for or treat individuals with mental illness.
As noted, the original mandate of the PAIMI legislation was to protect the mentally ill in institutions from abuse and neglect. Over time, a series of court cases (Lessard v. Schmidt, O’Connor v. Donaldson, Wyatt v. Stickney) and Congressional acts expanded the focus to disability rights across hospitals and into community settings.51,52,53
What PAIMI legislation did not do was instruct these groups to advocate for individuals who either refuse to take psychiatric medication, want to stop medication, or are unable to cooperate with recommended treatment because they lack the capacity or insight due to their mental illness. Over the years since the enactment of this law, disability rights groups have dedicated significant time, effort, and resources towards helping people with severe mental illnesses avoid recommended treatment. Such actions can have deadly consequences.
In 2011, SAMHSA evaluated the PAIMI program and found that PAIMI program staff were not sufficiently trained or prepared to provide information on program issues. The evaluation also identified a potential for conflicting goal interests between SAMHSA and PAIMI, with little effort by the Center for Mental Health Services (CMHS) to resolve these conflicts. Stakeholders reported mixed results regarding the effectiveness of PAIMI services, noting that PAIMI primarily focused on psychiatric hospitals despite legislative requirements to serve individuals in both institutional and community-based settings. Additionally, SAMHSA observed a lack of provisions for the mentally ill.
Further, PAIMI does nothing to assist the mentally ill into needed treatment or hospitalization, and will often work against these measures.54 Additionally, PAIMI has been found to combat the adoption of Assisted Outpatient Therapy while forcing states to close state psychiatric hospitals despite the lack of available beds. Finally, PAIMI fails to meet legislative requirements primarily due to a lack of oversight from its parent organization, SAMHSA. This has led to several barriers erected in mental illness treatment by PAIMI, but equally concerning (and directly related to PAIMI’s function) is the lack of understanding and advocacy for treatment for the mentally ill in the community.55
Protection and advocacy groups funded through PAIMI legislation should be refocused to fulfill the specific tasks outlined in legislation and should not deviate from those defined responsibilities. Groups with staff lacking training or expertise in the care and treatment of severe mental illness should be barred from engaging in so-called advocacy that could worsen the disease and lead to tragic outcomes. Those that do participate in such activities should be defunded, and their resources redirected to a protection and advocacy group that will adhere to the law.
Conclusion
The consequences of deinstitutionalizing psychiatric hospital populations and not using civil commitment as a therapeutic tool when needed to compel mental health treatment are evident in American society. We have institutionalized the severely mentally ill in jails and prisons, left large numbers of mentally ill languishing for extended periods in hospital emergency departments awaiting psychiatric beds, or left them forgotten on the streets. Some disability rights activists cite a citizen’s “right to refuse treatment” when criticizing Civil Commitment. This criticism ignores the outcomes of this misguided psychiatric abolitionist movement, which include increased incarceration, increased hospitalization, and increased homelessness for the severely mentally ill.56 Legislation that limits the number of available beds for the severely mentally ill, narrows the definition of dangerousness, and restricts civil commitment must be reconsidered as legislators seek to revitalize American cities and implement President Trump’s Executive Order 14321.

Stay Informed
Sign up to receive updates about our fight for policies at the state level that restore liberty through transparency and accountability in American governance.